Heel pain... Plantar fascitiis - Sports Medicine Doctor Malta - Dr Danica Bonello Spiteri
Main menu:
Heel pain... Plantar fascitiis
Heel Pain... Plantar fascitiis (First published on vida magazine on October 2013)
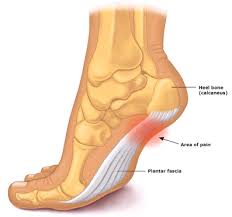
The plantar fascia is a thick tight band found on the sole of the foot. It originates from the heel (calcaneum bone), and stretches forward inserting into the toes so as to form a longitudinal arch, where it plays an important role in foot biomechanics.
This fascia provides support when walking as a means of shock absorption and when this is overused, it results in plantar fascitiis. The commonly injured area of the plantar fascia is its origin at the heel (calcaneum), where it results in an abnormal array of collagen fibres. There is no inflammation going on, as the process is similar to other tendionpathies, hence anti-
Plantar fascitiis arises from a number of causes, so management is directed towards the individual's cause, rather than one treatment for all.
Individuals with a low arch (pes planus) or high arch (pes cavus) of the foot are at an increased risk of developing plantar fascitiis. Pes planus places strain on the plantar fascia at the heel end, so the plantar fascia attempts to maintain a stable arch during each step of walking, running or jumping. Foot activities that cause the plantar fascia to be stretched, such as dancing and running are common in the athletic population. In the older population, incorrect foot biomechanics, excessive walking or inappropriate, non-
The plantar fascia dose not act in isolation, but in conjunction with other body parts, which, if not functioning well, may put additional strain. A good clincian should ensure good mobility in the ankle joint, assessing the calf, hamstring and buttock (gluteal) muscles for tightness, as these will all add towards increasing the strain on the plantar fascia by altering the foot biomechanics.
Increased body weight and work related weight bearing (carrying heavy loads repeatedly)are other issues that may need addressing.
The symptoms of plantar fascitiis are usually felt on the medial (inside) part of the heel and tend to be worst first thing in the morning when one gets out of bed. Exercise tends to make the pain lessen, only to become worse once one stops exercising. However, as time passes, the condition worsens and the pain is also present on simple standing up and worsens with activitiy.
The best way to view and diagnose plantar fascitiis is on ultrasound imaging, ideally performed by a specialist musculoskeletal radiologist, where the thickness of the fascia is also measured.
X-
Treatment for plantar fascitiis is individualised, depending on the causative factors. Any incorrect biomechanics of the feet need to be addressed, as well as any tightnesses in the calf, hamstring and quadriceps muscles. Avoidance of the aggravating activity, such as excessive walking or sudden increases in running distances need to be addressed.
Short term treatment includes stretching of the plantar fascia, ice and self massage with a golf ball or a frozen bottle by rolling it under the plantar fascia. For longer term management strengthening of the small muscles in the foot to help the arch support along with soft tissue therapy within the plantar fascia as well as the calf, hamstring and buttock muscles is helpful. Re-
More advanced treatment options may potentially include a corticosteroid injection, dry needling, extracorporeal shock wave therapy (ESWT) and platelet rich plasma (injecting blood products to enhance regeneration of the plantar fascia) are gaining popularity and increased effectiveness in this condition. Surgery is usually reserved as a last resort when all treatment has failed, but this is thought to have only a 'satisfactory' outcome.
The most important end note about plantar fascitiis is that the niggling heel pain is not ignored when it is in the initial stages, but medical attention is sought from the outset, so as to prevent it becoming a more chronic debilitating condition that is harder to treat.

For direct contact or to book a consultation please send an email on:
drdanica@sportsmedicinemalta.com