To X-ray or not to X-ray? - Sports Medicine Doctor Malta - Dr Danica Bonello Spiteri
Main menu:
To X-ray or not to X-ray?
To X-
Last month we dealt with the presenting scenario of back pain. This month we will deal with medical imaging in relation to back pain. It is not uncommon for a client seen in clinic to demand some form of imaging, namely x-
When a person presents with back pain, a detailed history and clinical examination often provides enough information for the specialist to make the diagnosis and start treatment. The history, which is the story the client tells, and the examination of the back will provide information about the function of the lower back and related structures that may be attributing to the back pain.
On the other hand, an x-
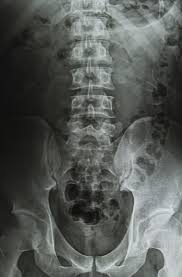
Imaging any person over the age of 30years old will show ‘degenerative’ changes within the back, and these are often age related changes, or normal wear and tear and do not necessarily mean that they are the actual cause of the back pain. This is often incorrectly called ‘degenerative disc disease’, and clients are labeled as such, and they believe this is the cause of their back pain. Degenerative changes in the back include decreasing disc space and some bony outgrowths from the vertebral bones, known as osteophytes (part of the picture of osteoarthritis). Such changes occur in everyone as we grow older, and are similar to the wrinkling and grey hair that occurs in all of us, so they are not a ‘disease’.
A good clinician should not be treating the changes seen on the x-
Due to time restraints and/or lack of adequate clinical skills in performing a detailed back examination, it is sometimes easier for a clinician to skip/skim through the examination and just write a piece of paper to request a scan. Once the scan returns as normal, the client may be waived off as having nothing ‘wrong’ with their backs, hence the client is once again at a loss.
On the other hand, if the scan comes back as abnormal, it may lead to more investigations, procedures, costs and risks to the client, all of which may be unrelated to the back pain, so this may also distress the client further, whilst going away from the actual back pain.
Unfortunately, in medical school, there is a lack of understanding and teaching about musculoskeletal conditions, including low back pain, hence a lack of clinical examination skills and understanding about the lower back. However, the increasing awareness about musculoskeletal medicine in Malta is changing, and will hopefully avoid unnecessary imaging being carried out on the wrong clients.
For direct contact or to book a consultation please send an email on:
drdanica@sportsmedicinemalta.com